Study reveals how persistent lung illness develops after recovery from COVID-19
The outcomes of the study were published in the ‘Journal of Clinical Investigation’
NEW DELHI — Short-term lung illness can cause long-term lung damage, according to a recent study.
The findings of this research were published in the ‘Journal of Clinical Investigation.’
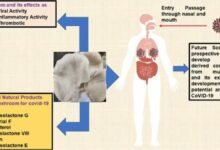
In some cases, the most dangerous part of a viral respiratory disease occurs after the virus has been eliminated from the body.
Severe infection results in organ damage & even death
Destructive processes that begin during an infection reach a peak in the weeks following the virus’s defeat, resulting in organ damage that can lead to chronic sickness or death.
Following an initial bout of COVID-19, some persons experience a chronic cough, trouble breathing, and shortness of breath, all of which are symptoms of ongoing lung damage.
Researchers uncover information about protein called IL-33
Washington University School of Medicine researchers in St. Louis have uncovered new information about how lung damage occurs following a respiratory infection.
They observed that infection causes the expression of a protein called IL-33, which is required for lung stem cells to overgrow into air gaps, resulting in increased mucus production and inflammation.
The data showed possible intervention sites to prevent viral infections from causing persistent lung damage.
Acute respiratory infections have long been known to cause chronic lung disease.
Children who have been hospitalized with the respiratory syncytial virus, for example, are two to four times more likely to develop asthma that lasts for years, if not a lifetime.
Exact mechanism causing chronic condition unknown
However, the exact mechanism by which an acute respiratory infection causes the chronic condition is unknown, making it challenging to design medications to prevent or treat it.
Holtzman and colleagues tested mice infected with the Sendai virus, including first author Kangyun Wu, PhD, an instructor of medicine.
Sendai does not cause major disease in humans, but it does infect other animals, particularly mice, and produces respiratory infections that are similar to those seen in humans.
Lung tissues from uninfected mice used for study
The researchers compared lung tissues from infected mice to lung tissues from uninfected mice 12 and 21 days following infection with the Sendai virus.
AT2 cells are limited to air sacs, while basal cells take over small airways and air sacs. Some of the newly formed basal cells produce mucus, while others secrete molecules that attract immune cells to the lungs.
Overall, the process leaves the lungs with reduced air room, increased mucus, and persistent inflammation, all of which make breathing difficult.
Further research revealed that the protein IL-33 is involved in this process. In the absence of stress or injury, IL-33 rises in the nucleus of lung stem cells and aids in the repair of damaged barriers.